Appointment Preparation
Contact Lens Wearers
Patients should refrain from wearing contact lenses for an extended period leading up to their pre-op appointment.
Soft contact lenses: 1-2 weeks
Hard contact lenses: 2-3 weeks
Historically, patients should refrain from wearing hard contacts for 1 week per every decade worn.
Realistically, these patients usually must refrain from using hard lenses for 2-3 weeks.
DES | Dry Eye Syndrome
Dry eye symptoms and ocular surface should be assessed and optimized prior to pre-op appointment.
Regimen should be continued post-operatively
- Pause for the first 1-2 weeks after surgery if multi-use drop bottles are used.
(prevent contamination)
Relevant Ocular History
Refractive History
Surgery
Name of procedure
And complications encountered
Obtain original
- Refraction
- Keratometry readings
Manifest Refraction (MR) history
- Stable vs changing
Since refractive surgery, prior to cataract onset
Evaluate current topography & tomography
- To confirm patient reported history.
Astigmatism + Refraction
Read most recent glasses prescription via lensometer.
Myopic + Hyperopic Changes
Myopic shift:
Assess NSC as potential etiology.
Hyperopic shift:
Check for clinically significant macular pathologies via OCT.
(eg, edema, retinoschesis, central serous retinopathy.)
Intraocular History
Increased posterior capsule fragility
→ Increased risk of intraoperative break.
- Intravitreal injections
- Scleral buckle
- Vitrectomy
- Intraocular silicone
Nystagmus
General anesthesia recommended
- Reduces risk of intraoperative challenges.
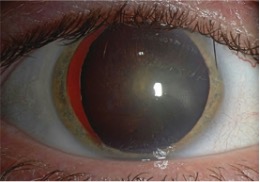
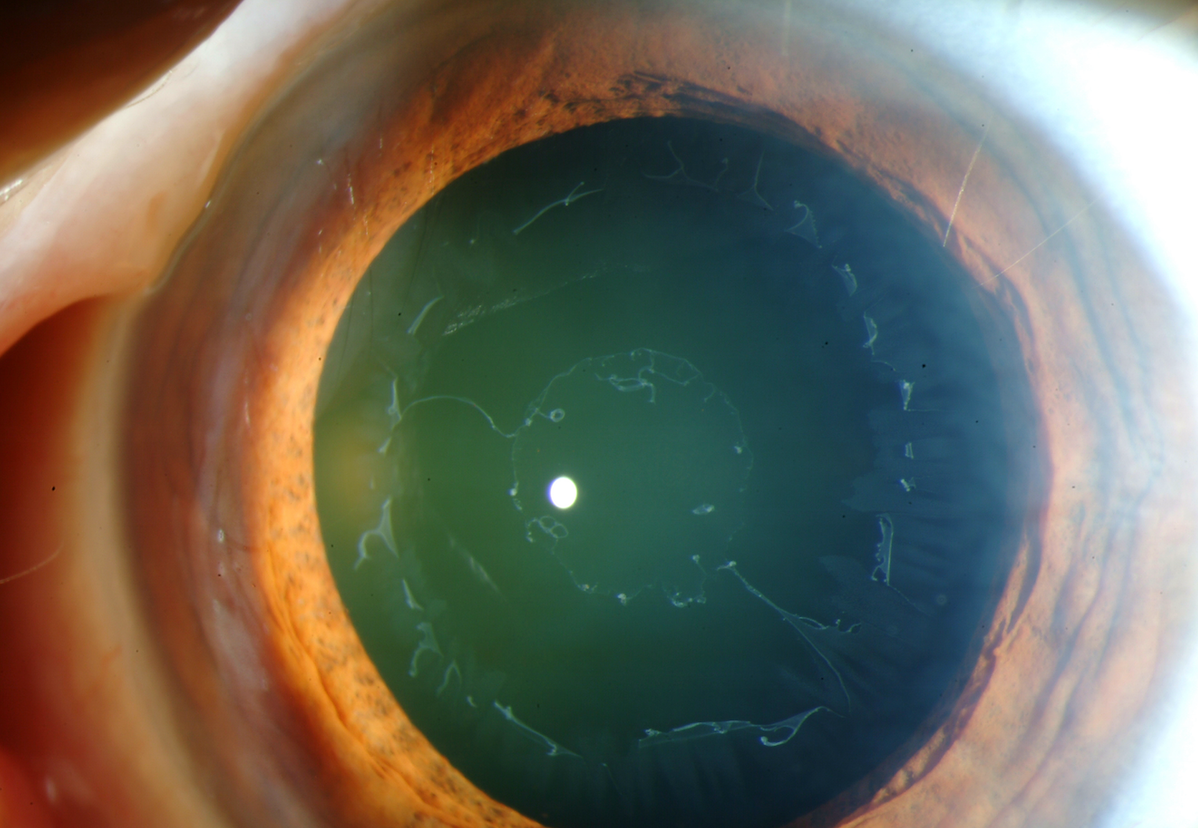
Disease History & Zonulopathy Asessment
Initial zonulopathy evaluation should be done in a non-dilated eye
Cycloplegics increase zonular tension and cause a falsely reassuring exam.
Ocular Trauma
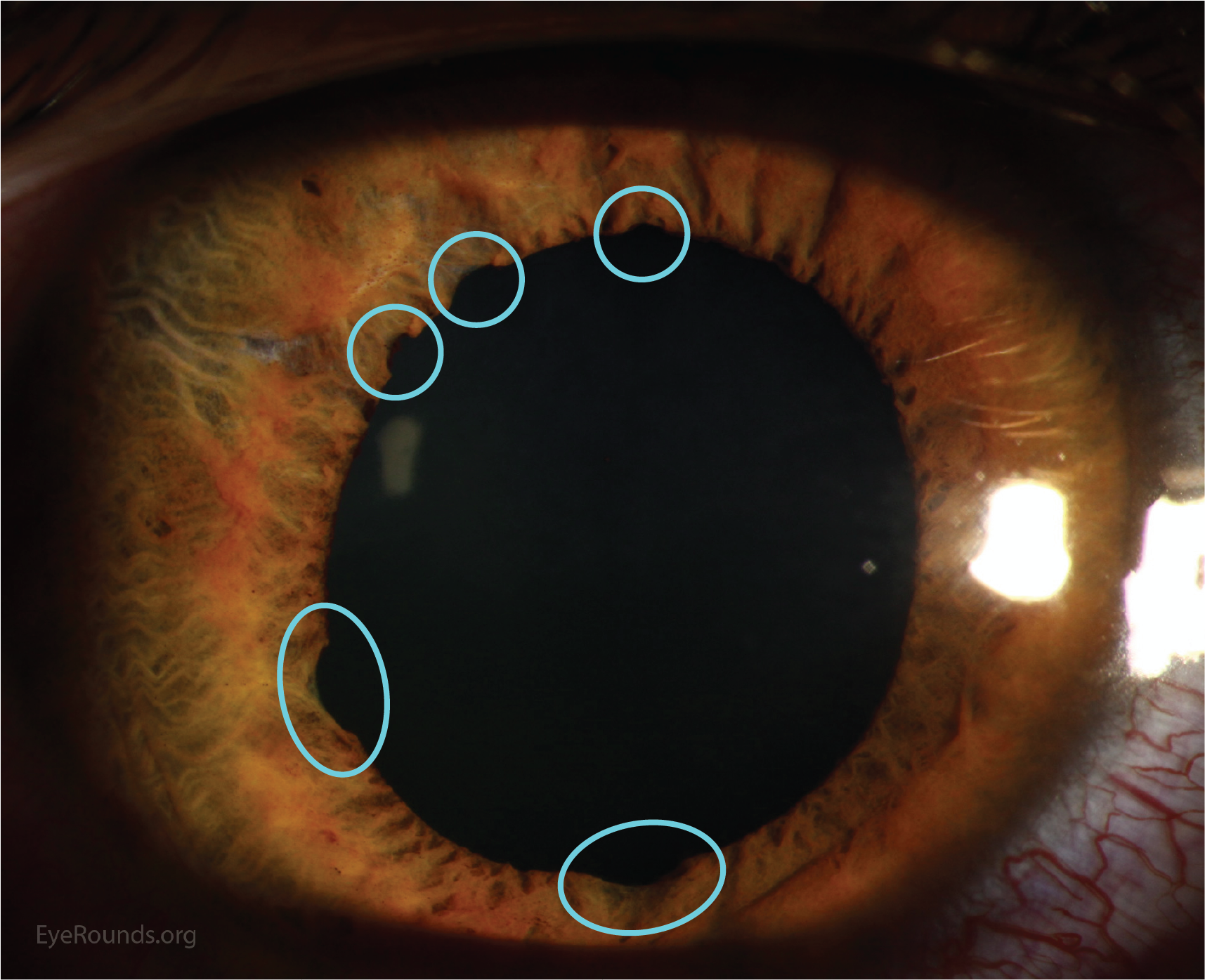
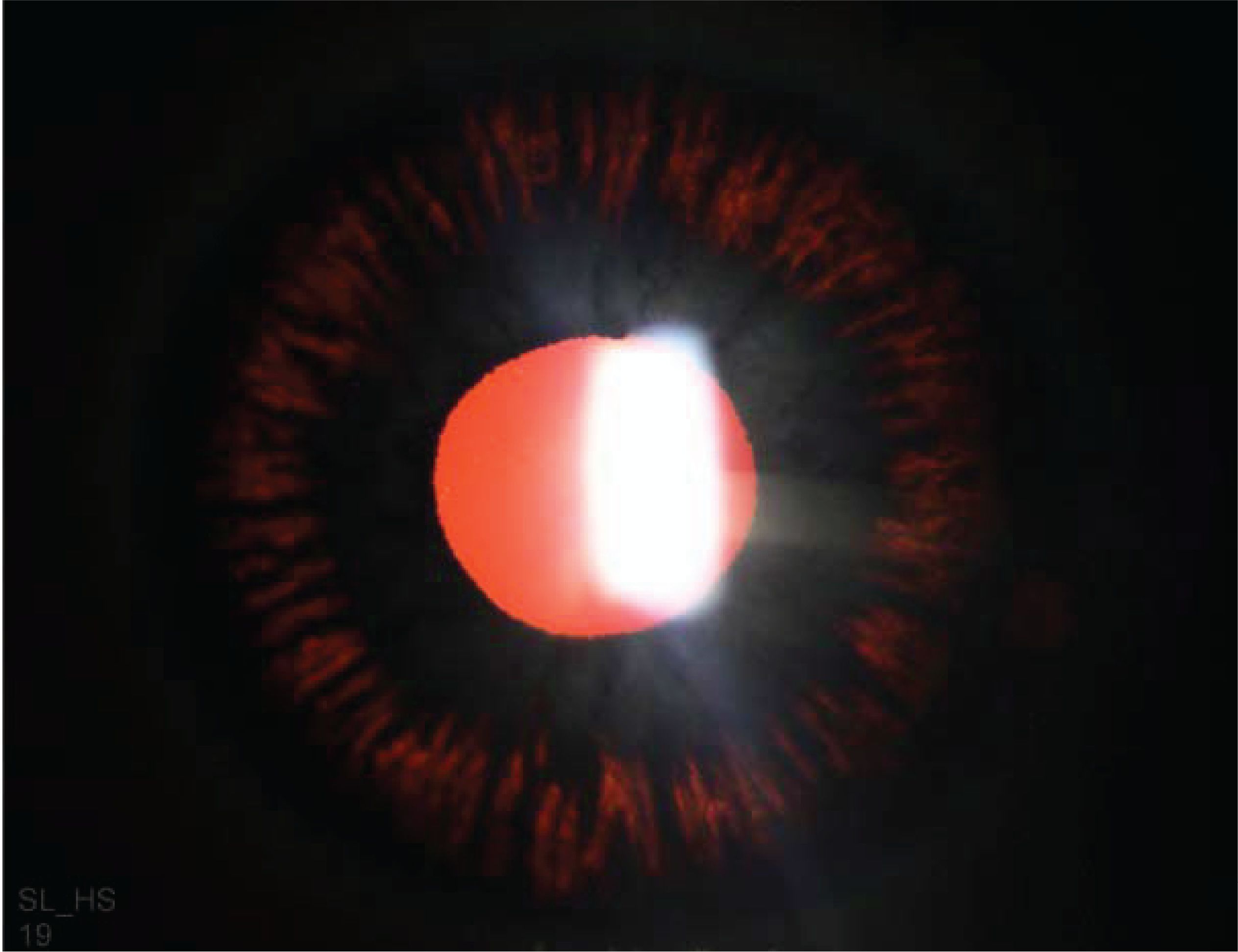
Pigmentary Dispersion Syndrome
- Mid-peripheral TIDs.
- Result of concave iris.
Uveitis
- 3-6 months of quiet and controlled inflammation prior to surgery.
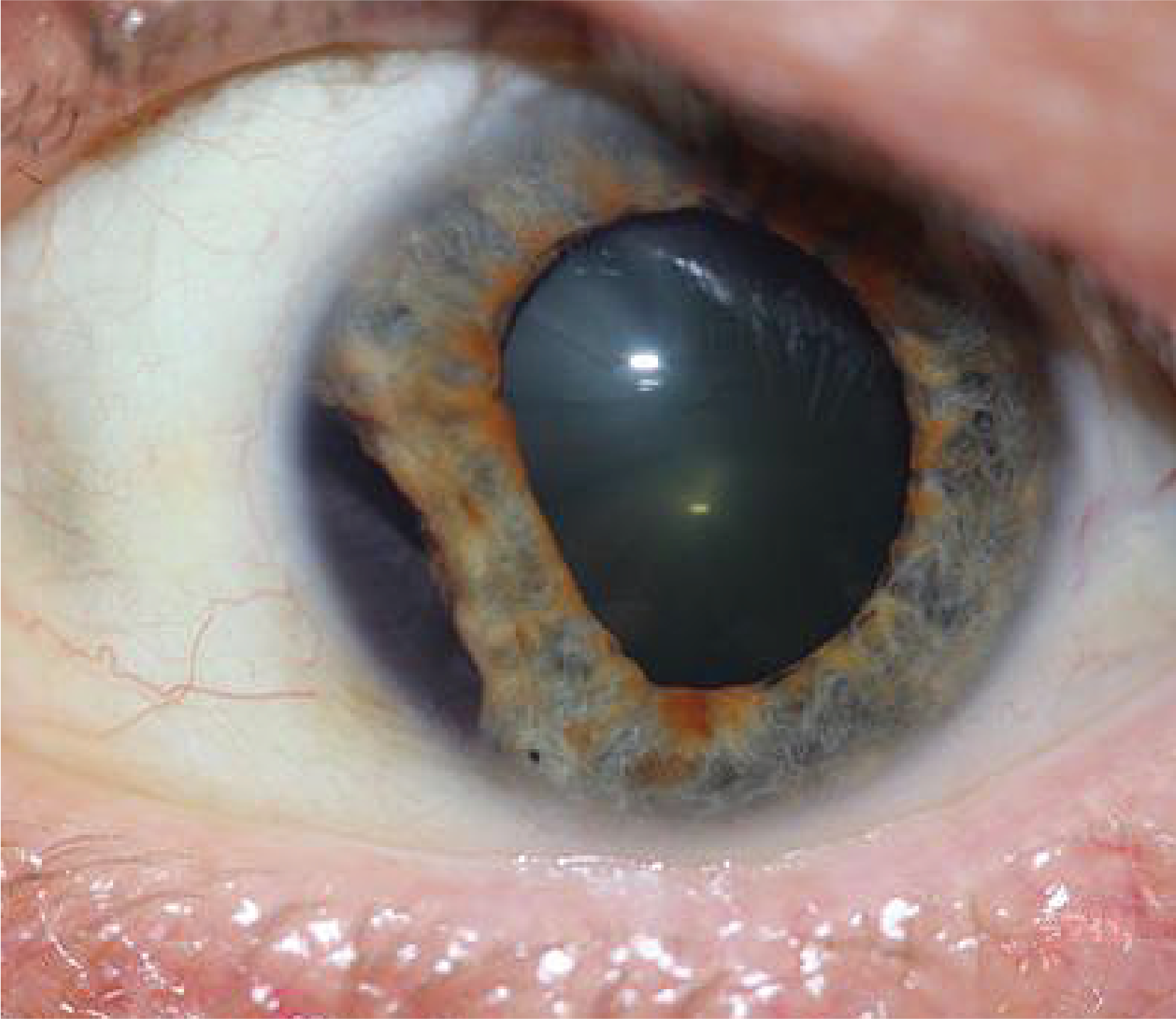
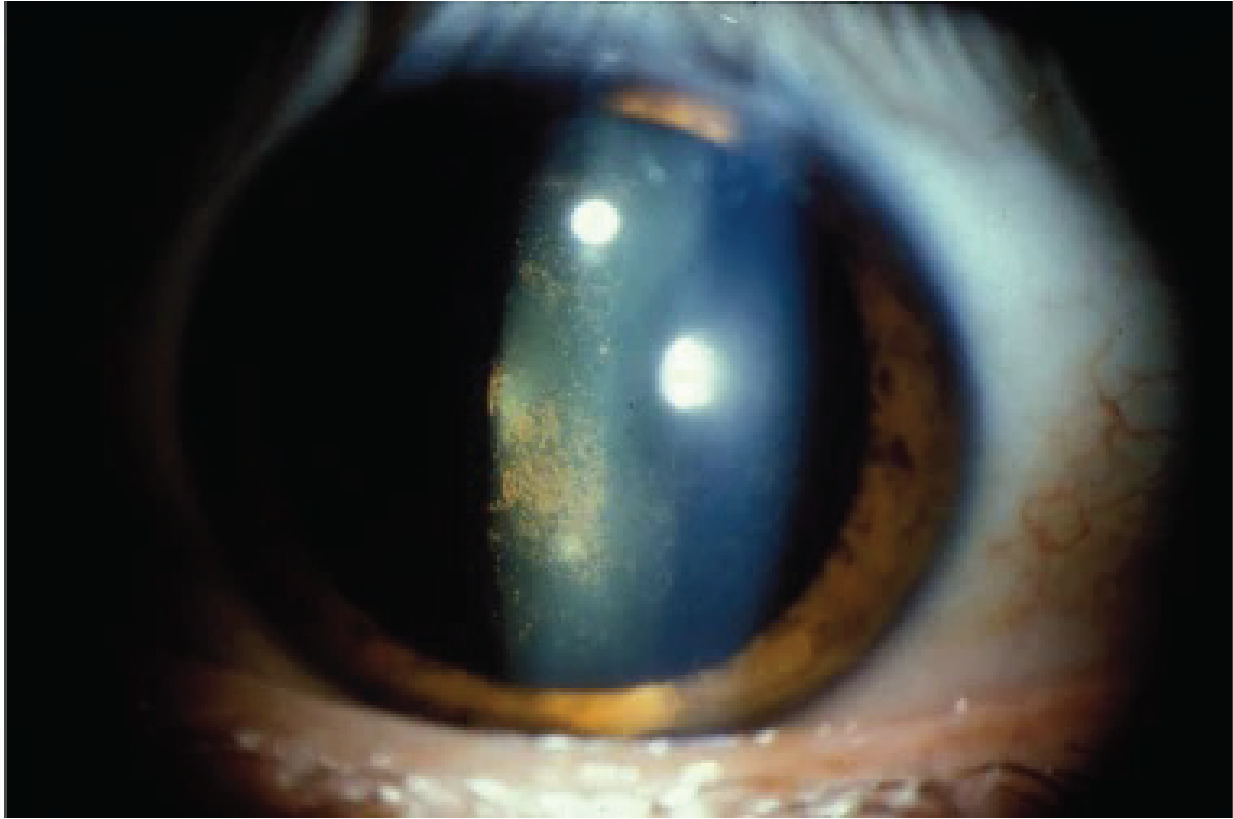
Pseudoexfoliation Syndrome
- Pupillary border TIDs.
- Causes zonulopathy.
Additional Exam Asessments
A thorough exam assessing all ocular co-morbidities reduces the chances of complications and ensures optimized outcomes.